Your gut does far more than digest food. It influences immunity, metabolism, mood, sleep, skin health, and even inflammation levels. Inside your digestive tract lives a vast ecosystem of bacteria, fungi, and viruses known as the gut microbiome. When this ecosystem is balanced, it supports health. When disrupted — a state often called gut dysbiosis — a wide range of symptoms may appear.
In this guide, we explain 10 common signs of an unhealthy gut, what they may mean, and science-based ways to improve gut health.
Why Gut Health Matters
Research over the past two decades has linked gut imbalance with:
- Digestive disorders (IBS, constipation, diarrhea)
- Immune dysfunction
- Mood and stress regulation
- Skin conditions
- Metabolic health
- Systemic inflammation
While the gut is not the sole cause of these conditions, it is often a significant contributing factor.
10 Signs Your Gut May Be Unhealthy
1. Persistent Gas and Bloating
Some gas is normal. However, frequent bloating, pressure, or discomfort may suggest:
- Excess fermentation
- Food intolerance
- Altered gut bacteria
- Small intestinal bacterial overgrowth (SIBO)
Patient example:
A 34-year-old office worker experienced bloating every afternoon despite “healthy eating.” Evaluation revealed lactose intolerance and irregular meal timing. Symptoms improved after dietary adjustments.
2. Constipation
Constipation may be associated with:
- Low fiber intake
- Dehydration
- Slow gut motility
- Microbiome imbalance
Studies show people with constipation sometimes have lower levels of beneficial bacteria such as Bifidobacterium.
When to seek care:
If constipation lasts more than 2–3 weeks or includes pain, bleeding, or weight loss.
3. Frequent Diarrhea
Chronic diarrhea may indicate:
- Infection
- Food intolerance
- IBS
- Inflammatory bowel disease (IBD)
- Microbial imbalance
Severe or persistent diarrhea can also disrupt beneficial bacteria.
4. Mood Changes (Anxiety, Low Mood, Irritability)
The gut–brain axis links digestion and emotional health. Gut microbes influence neurotransmitters and inflammation.
Evidence suggests gut imbalance may contribute to:
- Anxiety
- Stress sensitivity
- Low mood
Important note: Mood disorders are complex. Gut health is one factor among many.
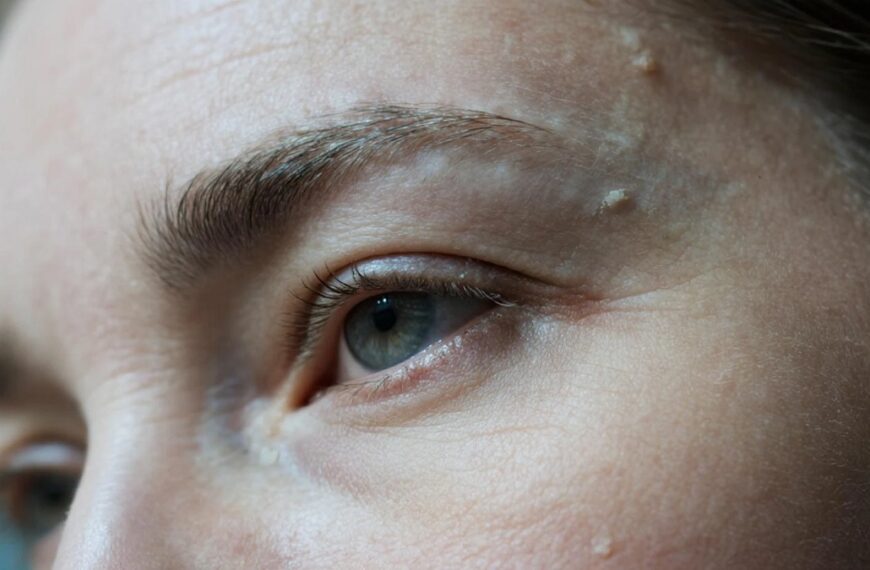
5. Skin Problems (Acne, Eczema, Rosacea)
Inflammatory skin conditions sometimes coexist with gut issues.
Possible mechanisms:
- Immune activation
- Inflammation
- Altered gut permeability
Patient example:
A teenager with acne and frequent digestive discomfort saw skin improvement after managing a high-sugar diet and addressing constipation.
6. Strong Sugar Cravings / High-Sugar Diet
Diets high in refined sugars and ultra-processed foods can:
- Reduce microbial diversity
- Promote pro-inflammatory bacteria
- Increase inflammation markers
Reducing added sugar often improves both energy stability and digestion.
7. Unexplained Weight Changes
Gut imbalance may influence:
- Appetite hormones
- Nutrient absorption
- Insulin sensitivity
However, weight change always requires medical evaluation to exclude thyroid, hormonal, or metabolic causes.
8. Poor Sleep or Chronic Fatigue
Gut health affects sleep through:
- Serotonin and melatonin pathways
- Inflammation
- Blood sugar regulation
Poor sleep also negatively affects the microbiome — creating a two-way cycle.
9. Autoimmune Conditions
Emerging research suggests gut barrier integrity and microbial balance may influence immune regulation. While not a direct cause, gut dysfunction may be a modifying factor.
10. Food Intolerances
Food intolerances (not allergies) may present as:
- Bloating
- Gas
- Diarrhea
- Nausea
- Fatigue
Common triggers include lactose, FODMAPs, gluten (non-celiac sensitivity), and certain additives.
How to Improve Gut Health
1. Manage Stress
Chronic stress can alter gut motility, increase inflammation, and affect microbial balance.
Helpful strategies:
- Regular physical activity
- Breathing exercises
- Mindfulness
- Adequate rest
2. Exercise Regularly
Moderate aerobic exercise has been associated with:
- Greater microbial diversity
- Improved bowel function
- Reduced inflammation
Aim for 150 minutes per week.
3. Prioritize Sleep
Target 7–9 hours per night. Sleep deprivation is linked with microbiome disruption and increased cravings.
4. Stay Hydrated
Adequate fluid intake supports:
- Stool consistency
- Gut lining protection
- Digestive efficiency
5. Eat Slowly and Chew Well
Proper chewing aids digestion and may reduce bloating.
6. Consider Prebiotics and Probiotics (With Guidance)
- Prebiotics feed beneficial bacteria (fiber-rich compounds)
- Probiotics introduce live beneficial microbes
Not everyone benefits from supplements. For example, some SIBO patients worsen with probiotics.
Consult a qualified clinician before starting.
7. Identify Food Triggers
An elimination approach may help uncover intolerances.
Work with a healthcare provider if symptoms are severe or unclear.
8. Improve Dietary Quality
A gut-supportive diet emphasizes:
- Fiber-rich plant foods
- Diverse vegetables
- Lean proteins
- Fermented foods (if tolerated)
- Reduced ultra-processed foods
Best Foods for Gut Health
High-Fiber Foods
Support beneficial bacteria and stool regularity.
Examples:
- Legumes
- Oats
- Vegetables
- Fruits
- Seeds
Evidence: High-fiber diets are consistently associated with greater microbial diversity and lower inflammation risk.
Fermented Foods
Provide live microbes and beneficial metabolites.
Examples:
- Yogurt with live cultures
- Kefir
- Sauerkraut
- Kimchi
- Miso
Evidence: Regular intake may improve microbial composition and digestive symptoms in some individuals.
Garlic and Onions
Contain natural prebiotic fibers (inulin, FOS).
Polyphenol-Rich Foods
Feed beneficial bacteria.
Examples:
- Berries
- Green tea
- Cocoa
- Olive oil
About Collagen and Bone Broth
Collagen’s direct benefit to gut health remains inconclusive. While generally safe, claims should be viewed cautiously.
Signs Your Gut May Be Healing
Patients often report:
- More regular bowel movements
- Reduced bloating
- Improved energy
- Better sleep
- Clearer skin (in some cases)
Healing timelines vary widely depending on diet, stress, sleep, and underlying conditions.
When to See a Healthcare Professional
Seek medical advice if you experience:
- Persistent diarrhea or constipation
- Blood in stool
- Unintentional weight loss
- Severe abdominal pain
- Ongoing fatigue
- Symptoms lasting > 2–4 weeks
Frequently Asked Questions
What is the gut?
The gastrointestinal (GI) tract runs from the mouth to the anus and includes the stomach, small intestine, and large intestine.
What are symptoms of gut inflammation?
May include:
- Abdominal pain
- Diarrhea
- Blood in stool
- Fatigue
- Weight loss
These symptoms require medical evaluation.
What does a healthy gut feel like?
Typically:
- Regular bowel movements
- Minimal bloating
- Comfortable digestion
- Stable energy
How do you “get rid of bad bacteria”?
Rather than eliminating bacteria, focus on restoring balance:
- Improve diet quality
- Increase fiber
- Manage stress
- Address infections if present
How can I improve gut health naturally?
- Eat diverse plant foods
- Stay hydrated
- Exercise regularly
- Sleep well
- Limit ultra-processed foods
What are the most common signs of an unhealthy gut?
Typical signs include bloating, excessive gas, constipation, diarrhea, food intolerances, fatigue, sleep disturbances, skin issues, mood changes, and unexplained weight fluctuations.
Can gut health affect mental health?
Yes. The gut and brain communicate through the gut–brain axis. Imbalances in gut bacteria may influence mood, stress responses, and anxiety levels.
How long does it take to heal the gut?
Gut recovery varies. Some people notice improvement within weeks after dietary and lifestyle changes, while others may require several months depending on underlying conditions.
What foods help improve gut health?
Fiber-rich foods, fermented foods (like yogurt and kefir), vegetables, fruits, legumes, and polyphenol-rich foods support a healthy gut microbiome.
Are probiotics necessary for gut health?
Not always. Many individuals benefit from improving diet first. Probiotics may help certain patients but should be selected with professional guidance.
When should I see a doctor for gut symptoms?
Seek medical evaluation if symptoms persist beyond 2–4 weeks, worsen, or include red flags such as blood in stool, severe pain, or weight loss.
Can stress damage gut health?
Chronic stress can alter gut motility, increase inflammation, and disrupt microbiome balance, contributing to digestive discomfort.
Is bloating always a sign of gut disease?
No. Occasional bloating is common. Persistent or painful bloating may require assessment for intolerances, IBS, or microbial imbalance.
Evidence-Informed Perspective
Gut health research is rapidly evolving. While associations are strong, many findings show correlation rather than direct causation. Personalized assessment remains essential.
About NFH Clinic
At NFH Clinic, we take a patient-centered, evidence-guided approach to digestive health. If you struggle with persistent gut symptoms, our clinicians can help evaluate diet, lifestyle, and medical factors contributing to imbalance.