Overview (Clinically Reviewed | NFH Clinic)
Iron deficiency occurs when the body lacks sufficient iron to produce healthy red blood cells and hemoglobin. This reduces oxygen delivery to tissues, leading to fatigue, weakness, pale skin, shortness of breath, dizziness, headaches, brittle nails, hair thinning, cold intolerance, and poor concentration.
Early symptoms are often subtle and easily mistaken for stress or lack of sleep. Untreated iron deficiency can progress to iron deficiency anemia, increasing the risk of heart strain, pregnancy complications, reduced immunity, and impaired cognitive performance.
Common causes include inadequate dietary iron intake, blood loss (heavy menstruation, gastrointestinal bleeding), pregnancy, malabsorption (e.g., celiac disease), and chronic illness.
Seek medical evaluation if symptoms persist. Diagnosis is confirmed via blood tests such as serum ferritin, hemoglobin, transferrin saturation, and complete blood count (CBC).
Treatment options may include dietary correction, oral iron supplementation, or intravenous iron under clinical supervision.
Medical Disclaimer: This content is for educational purposes and does not replace professional medical advice. Always consult a qualified healthcare provider.
Quick Facts: Iron Deficiency Symptoms
| Category | Key Information |
|---|---|
| Condition | Iron Deficiency / Iron Deficiency Anemia |
| Primary Mechanism | Reduced hemoglobin → decreased oxygen transport |
| Most Common Symptoms | Fatigue, weakness, pale skin |
| Neurological Signs | Dizziness, headaches, brain fog |
| Physical Indicators | Brittle nails, hair loss, cold hands/feet |
| Breathing/Cardiac | Shortness of breath, rapid heartbeat |
| At-Risk Groups | Women, pregnancy, children, vegetarians, chronic disease |
| Potential Complications | Anemia, heart stress, pregnancy risks |
| Diagnosis | Serum ferritin, hemoglobin, CBC |
| Treatments | Diet improvement, iron supplements, IV iron |
| When to Seek Care | Persistent fatigue, breathlessness, unexplained weakness |
Iron Deficiency Symptoms: Causes, Diagnosis & Treatment
Iron deficiency is the most common nutritional deficiency worldwide and a leading cause of iron deficiency anemia. It occurs when the body lacks sufficient iron to produce hemoglobin — the protein in red blood cells responsible for carrying oxygen to tissues. Because oxygen delivery is essential for energy production, brain function, and organ performance, iron deficiency can affect nearly every system in the body.
Early symptoms are often subtle and develop gradually. Patients may experience persistent fatigue, reduced exercise tolerance, headaches, hair thinning, brittle nails, or difficulty concentrating. As deficiency progresses, more pronounced signs may appear, including pale skin, shortness of breath, heart palpitations, dizziness, restless legs, or unusual cravings such as ice (pagophagia). In severe cases, untreated iron deficiency anemia can strain the cardiovascular system and impair daily functioning.
Diagnosis requires laboratory testing. Ferritin is the most reliable marker of iron stores, and low ferritin confirms iron deficiency in most cases. Hemoglobin may remain normal in early stages, which is why testing ferritin is essential when symptoms are present.
Treatment depends on severity and underlying cause. Oral iron supplements are typically first-line therapy for mild to moderate deficiency. Intravenous (IV) iron infusions are recommended when oral iron is ineffective, poorly tolerated, or when rapid correction is medically necessary. Full recovery involves not only restoring hemoglobin but also replenishing iron stores and identifying the source of iron loss.
Long-term prevention requires monitoring ferritin levels, maintaining adequate dietary intake, and evaluating persistent or recurrent deficiency — particularly in men and postmenopausal women, where iron deficiency may signal gastrointestinal bleeding or other serious conditions.
With proper diagnosis, targeted treatment, and appropriate follow-up, iron deficiency is highly treatable and reversible. Early recognition prevents complications and restores energy, cognitive performance, and overall quality of life.
Why Iron Deficiency Deserves Serious Attention
Iron deficiency is the most common nutritional deficiency worldwide and one of the leading causes of anemia across all age groups. While many people associate it only with “feeling tired,” iron deficiency is far more complex. It affects oxygen transport, immune regulation, neurological function, cardiovascular performance, pregnancy outcomes, and cognitive health.
In clinical practice, iron deficiency often develops gradually. Patients frequently normalize symptoms such as fatigue, hair shedding, or poor concentration—sometimes for years—before diagnosis. By the time it is detected, iron stores may be severely depleted.
This in-depth guide explains:
- What iron deficiency is
- Why symptoms occur
- Early vs. late warning signs
- Laboratory testing and interpretation
- Clinical case examples
- Evidence-based treatment options
- When symptoms require urgent care
This article is written in a medical authority tone and structured to provide patient-centered clarity, while reflecting standards consistent with leading academic health institutions.
What Is Iron Deficiency?
Iron is an essential mineral required for:
- Hemoglobin production (oxygen transport in red blood cells)
- Myoglobin function (oxygen storage in muscle)
- Mitochondrial energy production
- DNA synthesis
- Immune function
- Neurotransmitter metabolism
When the body’s iron stores decline, three progressive stages typically occur:
1. Iron Depletion (Low Ferritin)
Iron stores are reduced, but hemoglobin may still be normal.
2. Iron-Deficient Erythropoiesis
The body begins struggling to produce healthy red blood cells.
3. Iron Deficiency Anemia
Hemoglobin drops below normal, impairing oxygen delivery to tissues.
Symptoms may begin before anemia appears, which is why ferritin testing is clinically important.
Why Iron Deficiency Causes Symptoms
The core mechanism behind most symptoms is reduced oxygen delivery.
Hemoglobin contains iron. Without adequate iron:
- Red blood cells carry less oxygen
- Tissues receive less oxygen
- Cells produce less energy
- Organs compensate by working harder
This leads to fatigue, paleness, shortness of breath, heart palpitations, neurological symptoms, and other systemic effects.
Early Iron Deficiency Symptoms (Often Overlooked)
Iron deficiency often presents subtly.
Explanation
Many patients initially report “just being tired.” However, this fatigue is not typical tiredness—it is physiologic energy impairment caused by insufficient oxygen at the cellular level.
Common Early Symptoms
- Persistent fatigue
- Reduced exercise tolerance
- Brain fog or difficulty concentrating
- Irritability
- Mild headaches
- Hair shedding
- Brittle nails
- Cold intolerance
Clinical Interpretation
At this stage, hemoglobin may still be within normal range. Ferritin is usually low. This phase is frequently missed unless iron studies are specifically ordered.
Extreme Fatigue and Weakness
Why It Happens
Iron is required to produce hemoglobin, which carries oxygen to muscles and organs. Low iron reduces oxygen delivery and ATP production in mitochondria.
Symptoms
- Overwhelming exhaustion
- Feeling weak even after rest
- Difficulty completing routine activities
- Reduced stamina
Case Example
A 32-year-old teacher reports feeling exhausted by midday despite adequate sleep. She stopped exercising due to fatigue. Her hemoglobin is borderline normal, but ferritin is 9 ng/mL (low). After iron supplementation, energy improves significantly within 8 weeks.
Evidence-Based Note
Studies show that treating iron deficiency—even without anemia—can significantly improve fatigue scores in premenopausal women.
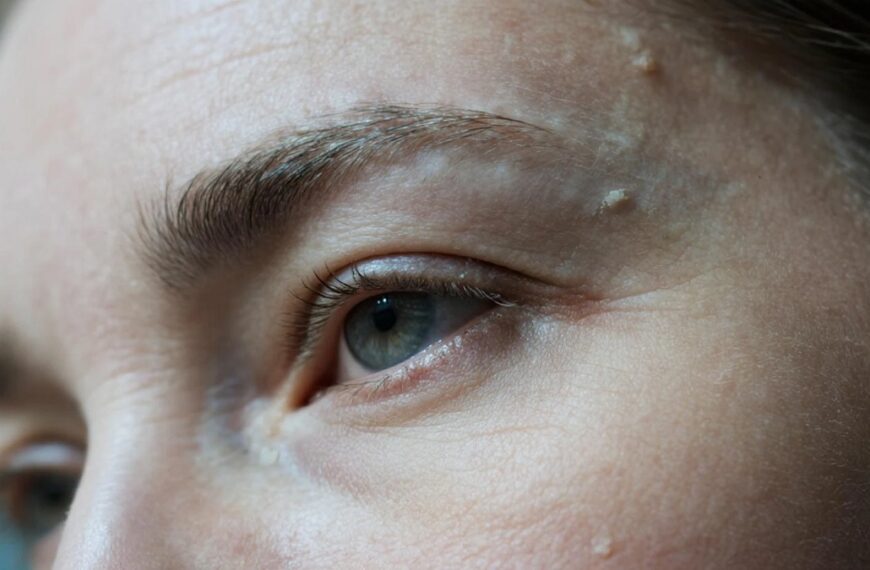
Pale Skin and Inner Eyelids
Why It Happens
Hemoglobin gives blood its red color. When hemoglobin decreases:
- Skin appears pale
- Inner eyelids (conjunctiva) lose pink tone
- Nail beds look lighter
Signs
- Facial paleness
- Pale gums
- Pale inner lower eyelid
Clinical Insight
Conjunctival pallor is a useful bedside clue but not diagnostic. Laboratory testing is required.
Shortness of Breath (Especially With Mild Activity)
Mechanism
Low hemoglobin reduces oxygen transport capacity. The body compensates by:
- Increasing breathing rate
- Increasing heart rate
Symptoms
- Winded climbing stairs
- Difficulty during mild exertion
- Needing frequent breaks
Clinical Caution
If shortness of breath occurs at rest or is accompanied by chest pain, urgent evaluation is necessary to rule out cardiac or pulmonary conditions.
Heart Palpitations and Tachycardia
Why the Heart Works Harder
When oxygen delivery decreases:
- Cardiac output increases
- Heart rate rises
- Palpitations may occur
Symptoms
- Racing heartbeat
- Pounding chest
- Irregular heartbeat sensation
Severe Risk
Untreated iron deficiency anemia can lead to:
- Left ventricular hypertrophy
- Heart failure (rare but possible in severe cases)
Headaches, Dizziness, and Brain Fog
Neurological Effects
The brain is highly oxygen-dependent. Reduced oxygen delivery can cause:
- Headaches
- Lightheadedness
- Difficulty concentrating
- Memory issues
Patient Example
A university student reports worsening focus and chronic headaches. Iron studies reveal low ferritin despite normal hemoglobin. Treatment leads to cognitive improvement.
Brittle or Spoon-Shaped Nails (Koilonychia)
Explanation
Iron deficiency can impair keratin structure.
Signs
- Thin nails
- Easy breakage
- Concave “spoon-shaped” appearance
Clinical Note
Koilonychia is uncommon but highly suggestive of chronic iron deficiency.
Hair Loss and Thinning
Why It Occurs
Iron supports rapidly dividing cells, including hair follicles.
Symptoms
- Diffuse hair shedding
- Thinning along scalp
- Reduced hair volume
Evidence Note
Low ferritin has been associated with telogen effluvium (diffuse hair loss). Restoration of iron stores may improve hair density.
Tongue and Mouth Changes
Glossitis
The tongue may become:
- Smooth
- Shiny
- Red
- Tender
Angular Cheilitis
- Cracks at corners of the mouth
Why It Happens
Rapidly dividing mucosal cells are sensitive to nutrient deficiencies.
Cold Hands and Feet
Mechanism
Reduced oxygen and altered circulation can cause:
- Persistent cold sensation
- Pale extremities
Pica (Unusual Cravings)
Definition
Pica is craving non-food substances.
Common Forms
- Ice (pagophagia)
- Dirt
- Clay
- Raw starch
Clinical Significance
Ice craving is strongly associated with iron deficiency. Symptoms often resolve after treatment.
Restless Legs Syndrome (RLS)
Explanation
Iron plays a role in dopamine metabolism in the brain.
Symptoms
- Urge to move legs
- Worse at night
- Relief with movement
Evidence-Based Note
Low ferritin (<50 ng/mL) has been associated with RLS. Iron therapy may improve symptoms.
Iron Deficiency in Children
Why It’s Critical
Iron is essential for brain development.
Signs in Children
- Poor appetite
- Irritability
- Delayed development
- Behavioral issues
- Learning difficulty
Long-Term Risk
Untreated iron deficiency in infancy may affect cognitive outcomes.
Iron Deficiency in Pregnancy
Iron needs increase substantially during pregnancy.
Risks Include
- Maternal fatigue
- Preterm delivery
- Low birth weight
- Postpartum depression
Routine screening is recommended in pregnancy.
Increased Infections and Immune Dysfunction
Iron influences immune cell activity.
Deficiency may result in:
- Increased infection susceptibility
- Slow wound healing
Severe Iron Deficiency Symptoms
If untreated, symptoms may escalate:
- Chest pain
- Fainting
- Severe shortness of breath
- Heart enlargement
- Cold extremities
Immediate medical evaluation is required in severe cases.
How Iron Deficiency Is Diagnosed
Diagnosis requires laboratory testing.
Core Tests
- Ferritin (best marker of iron stores)
- Serum iron
- Total iron-binding capacity (TIBC)
- Transferrin saturation
- Hemoglobin
- Mean corpuscular volume (MCV)
Key Interpretation
- Low ferritin confirms iron deficiency (unless inflammation present)
- Normal hemoglobin does not rule out deficiency
Common Causes of Iron Deficiency
Blood Loss
- Heavy menstrual bleeding
- Gastrointestinal bleeding
- Colon polyps
- Ulcers
- Hemorrhoids
Increased Needs
- Pregnancy
- Adolescence
- Endurance athletes
Reduced Absorption
- Celiac disease
- Gastric bypass
- Chronic inflammation
Poor Intake
- Restrictive diets
- Vegan diets without supplementation
Treatment: Evidence-Based Approach
Treatment must address both iron replacement and the underlying cause.
Oral Iron vs Intravenous (IV) Iron Therapy
Oral Iron vs IV Iron: Which Is Better?
| Category | Oral Iron Supplements | Intravenous (IV) Iron |
|---|---|---|
| Administration | Taken by mouth (tablets, capsules, liquid) | Given through a vein in a medical setting |
| Common Forms | Ferrous sulfate, ferrous gluconate, ferrous fumarate | Iron sucrose, ferric carboxymaltose, iron dextran |
| Best For | Mild to moderate iron deficiency | Moderate to severe deficiency, malabsorption, intolerance to oral iron |
| Speed of Hemoglobin Recovery | 6–8 weeks | 2–4 weeks (often faster in severe anemia) |
| Replenishing Iron Stores (Ferritin) | 3–6 months | Faster restoration of iron stores |
| Absorption Limitations | Reduced by food, calcium, tea, coffee | Bypasses gastrointestinal tract |
| Gastrointestinal Side Effects | Common (nausea, constipation, bloating, dark stools) | Minimal GI effects |
| Serious Risks | Rare (overdose risk if misused) | Rare allergic reactions; requires medical supervision |
| Convenience | Can be taken at home | Requires clinic visit |
| Cost Consideration | Lower cost | Higher cost; insurance coverage varies |
| When Preferred | First-line therapy in most patients | When oral therapy fails or rapid correction is needed |
- Cost of Iron Infusions: What Patients Should Know
- Does Insurance Cover IV Iron?
- How Many Iron Infusions Are Needed?
How Clinicians Decide Between Oral and IV Iron
In most patients, oral iron is first-line treatment due to safety, effectiveness, and cost efficiency. However, IV iron is medically appropriate in specific circumstances.
Oral Iron Is Preferred When:
- Iron deficiency is mild to moderate
- The patient tolerates supplements
- There is no significant malabsorption
- There is no urgent need for rapid correction
IV Iron Is Recommended When:
- Severe anemia is present
- Oral iron causes intolerable side effects
- There is inflammatory bowel disease or gastric surgery
- The patient is late in pregnancy and requires rapid correction
- There is ongoing blood loss
- Ferritin fails to improve despite compliance
Case Example 1 – Oral Iron Success
A 29-year-old woman with heavy menstrual bleeding presents with fatigue and ferritin of 8 ng/mL. Hemoglobin is mildly reduced. She begins oral ferrous sulfate. After 8 weeks, hemoglobin normalizes and symptoms improve. Ferritin restoration continues over 4 months.
This is the most common treatment pathway.
Case Example 2 – IV Iron Indication
A 54-year-old man with colon inflammation has ferritin of 5 ng/mL and severe anemia. Oral iron worsens gastrointestinal symptoms. IV iron sucrose is administered in two infusions. Hemoglobin improves within 3 weeks.
IV iron is medically appropriate when oral therapy is not tolerated or insufficient.
- Modern IV iron formulations have significantly lower allergic reaction rates than older formulations.
- Studies show alternate-day oral iron dosing may improve absorption and reduce side effects.
- Oral iron absorption improves when taken with vitamin C.
- In inflammatory conditions, oral iron absorption may be impaired due to elevated hepcidin levels.
Oral Iron Therapy
Typical Options
- Ferrous sulfate
- Ferrous gluconate
- Ferrous fumarate
Best Practices
- Take on empty stomach if tolerated
- Combine with vitamin C
- Avoid calcium at same time
Common Side Effects
- Constipation
- Nausea
- Dark stools
Intravenous Iron
Indicated when:
- Oral iron fails
- Severe anemia present
- Malabsorption exists
IV iron replenishes stores faster.
Cost of Iron Therapy: Insurance Coverage, Out-of-Pocket Expenses & What to Expect
Iron replacement therapy is medically necessary in many cases. However, the cost difference between oral iron supplements and intravenous (IV) iron infusions can be substantial, especially depending on insurance coverage.
Understanding potential costs helps patients make informed decisions in partnership with their healthcare provider.
Oral Iron Supplements: Cost Overview
Typical Cost (United States)
- Over-the-counter iron supplements: $5–$25 per month
- Prescription iron formulations: $10–$50 per month (depending on insurance)
Insurance Coverage
Most oral iron supplements:
- Are available over-the-counter (OTC)
- May not require insurance
- Are sometimes covered if prescribed
Because oral iron is inexpensive and widely available, it is typically the most cost-effective first-line treatment.
What Patients Should Know
- Generic ferrous sulfate is usually the most affordable option.
- Extended-release or “gentle” formulations may cost more.
- Insurance rarely requires prior authorization for oral iron.
Intravenous (IV) Iron Therapy: Cost Overview
IV iron therapy is more complex and significantly more expensive due to:
- Medication cost
- Infusion center fees
- Nursing supervision
- Facility charges
Typical Cost (United States)
Without insurance:
- $400 to $4,000 per infusion session
- Total treatment cost may range from $1,000 to $10,000 depending on formulation and number of sessions
With insurance:
- Patient responsibility depends on deductible, copay, and coinsurance
- Many patients pay 10–30% of total cost after deductible
Costs vary widely by:
- Geographic location
- Hospital-based vs outpatient infusion center
- Insurance plan structure
What Determines IV Iron Insurance Approval?
Insurance providers typically require documentation of:
- Confirmed iron deficiency (low ferritin or anemia)
- Failure or intolerance of oral iron
- Presence of a condition that impairs absorption
- Severe anemia requiring rapid correction
Prior authorization is commonly required.
Common Covered Indications
- Iron deficiency anemia
- Chronic kidney disease
- Inflammatory bowel disease
- Pregnancy with severe anemia
- Post-bariatric surgery malabsorption
Clinical Example: Insurance Approval Scenario
A 45-year-old patient with inflammatory bowel disease cannot tolerate oral iron due to severe gastrointestinal side effects. Ferritin is 6 ng/mL. Hemoglobin is significantly low.
After documentation of intolerance and lab confirmation, insurance approves IV iron therapy. The patient pays a specialist copay and coinsurance.
Hospital vs Independent Infusion Centers
Cost may differ depending on facility type:
Hospital-Based Infusion Center
- Higher facility fees
- Often higher total charges
- May offer integrated specialist care
Independent Outpatient Infusion Center
- Often lower cost
- More transparent billing
- Shorter wait times
Patients should confirm where the infusion will be administered.
Cost Comparison Table
| Treatment Type | Estimated Out-of-Pocket Cost (Without Insurance) | Insurance Coverage Likelihood |
|---|---|---|
| Oral Iron | $5–$50/month | High (minimal restrictions) |
| IV Iron (1 session) | $400–$4,000 | Moderate to High (with documentation) |
| Full IV Course | $1,000–$10,000 | Depends on deductible & approval |
Questions Patients Should Ask Their Insurance Provider
Before scheduling IV iron therapy, patients should ask:
- Is prior authorization required?
- What is my deductible?
- What percentage coinsurance applies?
- Is the infusion center in-network?
- How many infusions are covered per year?
This prevents unexpected billing.
High-Deductible Health Plans (HDHPs)
Patients with high-deductible plans may pay the full cost of IV iron until the deductible is met.
In these cases:
- Oral iron may be trialed first
- Payment plans may be available
- Some infusion centers offer self-pay discounts
International Cost Considerations
Outside the United States:
- Public healthcare systems often cover IV iron when medically indicated.
- Private insurance structures vary.
- Cost transparency is generally higher in nationalized systems.
Patients should consult local coverage policies.
Is IV Iron Worth the Cost?
IV iron may be cost-effective when:
- Oral therapy fails
- Symptoms are severe
- Rapid recovery is medically necessary
- Productivity loss from untreated anemia is high
For working adults, correcting severe anemia quickly may reduce:
- Missed work days
- Emergency department visits
- Cardiac complications
Financial Assistance Options
Patients may explore:
- Manufacturer assistance programs
- Hospital financial aid
- Payment plans
- Health Savings Accounts (HSA)
- Flexible Spending Accounts (FSA)
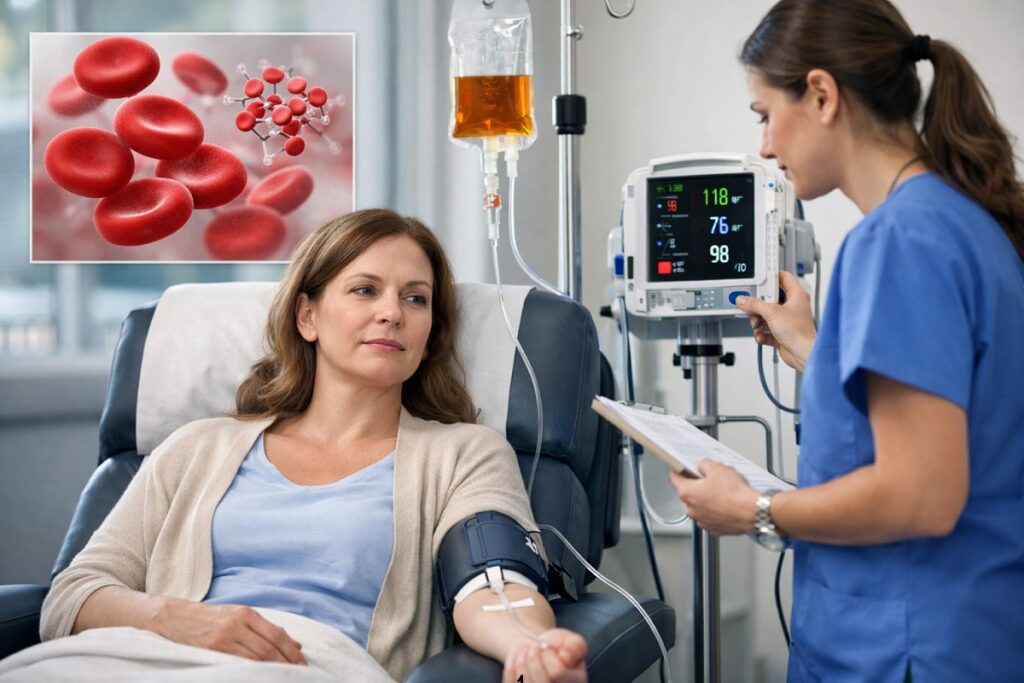
Iron Infusion Procedure: What to Expect Before, During, and After IV Iron Therapy
Intravenous (IV) iron therapy is a safe and effective treatment for moderate to severe iron deficiency and iron deficiency anemia, particularly when oral iron supplements are ineffective or poorly tolerated.
For many patients, the idea of receiving an infusion can cause anxiety. Understanding the process in detail helps reduce uncertainty and improve treatment adherence.
This section explains exactly what happens before, during, and after an iron infusion — from check-in to recovery.
Why Iron Infusions Are Prescribed
IV iron is typically recommended when:
- Oral iron causes significant gastrointestinal side effects
- Iron levels fail to improve despite compliance
- There is malabsorption (e.g., inflammatory bowel disease, bariatric surgery)
- Anemia is severe and requires rapid correction
- Late pregnancy requires faster repletion
- Ongoing blood loss prevents recovery with oral therapy
Unlike oral iron, IV iron bypasses the digestive system and delivers iron directly into the bloodstream.
Step 1: Pre-Infusion Evaluation
Explanation
Before scheduling an iron infusion, your clinician confirms iron deficiency through laboratory testing and ensures no contraindications exist.
Common Pre-Infusion Labs
- Ferritin
- Hemoglobin
- Serum iron
- Transferrin saturation
- Complete blood count (CBC)
In some cases, kidney function tests or inflammatory markers may also be checked.
Insurance Authorization
Most insurers require documentation of:
- Confirmed iron deficiency
- Trial or intolerance of oral iron
- Medical necessity
Prior authorization is common and may take several days to process.
Step 2: Arrival at the Infusion Center
Iron infusions are administered in:
- Hospital outpatient departments
- Independent infusion centers
- Specialty clinics
- Nephrology or hematology offices
What Happens at Check-In
- Vital signs are recorded (blood pressure, heart rate, temperature)
- Allergy history is reviewed
- Medication list is confirmed
- Consent is obtained
Patients are typically seated in a reclining infusion chair.
Step 3: IV Line Placement
A nurse inserts a small intravenous catheter into a vein in the arm.
What You May Feel
- Mild pinch during needle insertion
- Brief pressure sensation
Once the IV is secured, the infusion tubing is connected.
Step 4: The Iron Infusion Begins
The iron solution is diluted in saline and infused slowly.
Duration
Infusion time depends on formulation:
- Iron sucrose: 30–60 minutes
- Ferric carboxymaltose: 15–30 minutes
- Iron dextran: May require longer infusion time
Some formulations require multiple sessions spaced over days or weeks.
What You May Feel During the Infusion
Most patients tolerate IV iron well.
Common Mild Sensations
- Metallic taste
- Warmth
- Mild headache
- Slight nausea
- Temporary flushing
These symptoms are usually brief and resolve without intervention.
Monitoring During Infusion
Nursing staff monitor:
- Blood pressure
- Heart rate
- Signs of allergic reaction
- Patient comfort
Modern IV iron formulations have a low rate of serious allergic reactions, but monitoring is standard practice.
Rare but Serious Reactions
Although uncommon, severe reactions can include:
- Shortness of breath
- Chest tightness
- Rash or hives
- Severe hypotension
- Anaphylaxis
Infusion centers are equipped to manage allergic reactions immediately.
The risk of severe anaphylaxis with newer iron formulations is very low compared to older iron dextran products.
Step 5: Post-Infusion Observation
After the infusion is complete:
- The IV catheter is removed
- Pressure is applied to the site
- You may be observed for 15–30 minutes
Vital signs are rechecked before discharge.
After You Go Home
Most patients can resume normal activities immediately.
Possible Temporary Side Effects
- Mild fatigue
- Headache
- Muscle aches
- Darkened urine
- Injection site soreness
These typically resolve within 24–48 hours.
When to Contact Your Doctor After an Infusion
Seek medical attention if you experience:
- Persistent chest pain
- Difficulty breathing
- Severe rash
- Swelling of face or throat
- Fever above 101°F (38.3°C)
Delayed allergic reactions are rare but possible.
How Quickly Will You Feel Better?
Clinical improvement varies depending on severity.
Expected Timeline
- Energy improvement: 1–3 weeks
- Hemoglobin increase: 2–4 weeks
- Full symptom recovery: 4–8 weeks
Ferritin levels are typically rechecked 4–8 weeks after infusion.
How Many Iron Infusions Are Needed?
The number depends on:
- Degree of deficiency
- Body weight
- Type of formulation
- Ongoing blood loss
Some patients require:
- One large-dose infusion
- Two to five smaller infusions
Your clinician calculates the total iron deficit using standardized formulas.
Clinical Example: Severe Iron Deficiency
A 52-year-old woman presents with:
- Hemoglobin: 8.5 g/dL
- Ferritin: 4 ng/mL
- Symptoms: Severe fatigue, dizziness, palpitations
She receives two IV iron infusions spaced one week apart. Hemoglobin rises significantly within three weeks, and symptoms improve.
IV iron prevents prolonged functional impairment and reduces cardiovascular strain.
Is Iron Infusion Painful?
The infusion itself is not painful.
The only discomfort typically occurs during IV insertion. Most patients describe the experience as similar to receiving IV fluids.
Safety Profile of Modern IV Iron
Large clinical studies show:
- Serious allergic reactions are rare
- Gastrointestinal side effects are minimal
- Iron overload is unlikely when properly dosed
IV iron is considered safe when administered under medical supervision.
Advantages of Iron Infusion
- Faster correction of anemia
- Avoids gastrointestinal irritation
- Improved absorption in inflammatory conditions
- Fewer compliance issues
Disadvantages
- Higher cost
- Requires clinic visit
- Insurance authorization may be needed
- Rare allergic reactions
Common Questions About Iron Infusions
Can I drive myself home after an iron infusion?
Yes, unless you feel lightheaded or unwell.
Do iron infusions cause weight gain?
No. Iron itself does not cause weight gain.
Can I exercise after an infusion?
Light activity is acceptable the same day. Resume normal exercise as tolerated.
Will I need repeat infusions?
Possibly, if the underlying cause of deficiency persists.
When Iron Infusion Is Urgently Needed
Immediate treatment may be required if:
- Hemoglobin is dangerously low
- Cardiac symptoms develop
- Pregnancy complications arise
- Surgery is scheduled soon
In some cases, blood transfusion may be considered if anemia is life-threatening.
Long-Term Monitoring After Iron Infusion
Follow-up includes:
- Repeat hemoglobin
- Ferritin level
- Evaluation of underlying cause
- Ongoing prevention plan
Addressing the root cause prevents recurrence.
Final Clinical Perspective
Iron infusion therapy is a medically supervised, evidence-based treatment for iron deficiency and iron deficiency anemia. While oral iron remains first-line therapy, IV iron offers a safe and efficient alternative when rapid correction is necessary or oral treatment fails.
For many patients, iron infusion significantly improves quality of life, restores energy, and prevents long-term complications.
How Long Does Recovery Take?
- Symptom improvement: 2–4 weeks
- Hemoglobin normalization: 6–8 weeks
- Ferritin repletion: 3–6 months
Iron therapy should continue 3 months after normalization to rebuild stores.
Patient Case Example: Chronic Menstrual Blood Loss
A 38-year-old woman with heavy periods presents with:
- Fatigue
- Hair thinning
- Ice craving
Ferritin: 7 ng/mL
Hemoglobin: Mildly low
After iron therapy and gynecologic evaluation, symptoms resolve. Long-term management includes addressing menstrual blood loss.
How to Prevent Iron Deficiency
Prevention depends on identifying risk factors and ensuring adequate intake and monitoring.
1. Maintain Adequate Dietary Iron Intake
Iron exists in two forms:
Heme Iron (Best Absorbed)
- Red meat
- Poultry
- Fish
Non-Heme Iron (Plant Sources)
- Lentils
- Spinach
- Beans
- Tofu
- Fortified cereals
Enhance absorption by combining iron-rich foods with vitamin C (citrus, bell peppers).
Avoid consuming calcium supplements or tea/coffee at the same time as iron-rich meals.
2. Monitor High-Risk Populations
Routine screening is recommended for:
- Pregnant women
- Women with heavy periods
- Infants and toddlers
- Adolescents
- Endurance athletes
- Post-bariatric surgery patients
Early ferritin testing prevents progression to anemia.
3. Address Heavy Menstrual Bleeding
Women experiencing:
- Periods lasting longer than 7 days
- Passing large clots
- Needing double protection
Should seek gynecologic evaluation. Treating the source of blood loss prevents recurrent deficiency.
4. Evaluate Gastrointestinal Health
Adults over 40 with unexplained iron deficiency should undergo evaluation for:
- Colon polyps
- Ulcers
- Inflammatory bowel disease
- Colorectal cancer
Iron deficiency may be the first sign of occult bleeding.
5. Use Supplements Responsibly
Iron supplementation should be:
- Clinician-guided
- Monitored with follow-up labs
- Continued long enough to restore ferritin
Excess iron can cause toxicity. Self-diagnosing and self-supplementing is not recommended.
When to See a Doctor
Seek medical care if you experience:
- Persistent fatigue
- Shortness of breath
- Unexplained hair loss
- Heavy periods
- Black stools
- Chest pain
Iron deficiency may signal underlying gastrointestinal bleeding, especially in men and postmenopausal women.
Frequently Asked Questions
What are the first signs of iron deficiency?
Early iron deficiency often presents with subtle symptoms before anemia develops. Common early signs include:
- Persistent fatigue
- Reduced exercise tolerance
- Brain fog
- Headaches
- Hair thinning
- Brittle nails
Iron deficiency can exist even when hemoglobin levels are normal. Ferritin testing is often required to detect early depletion.
Can you have iron deficiency without anemia?
Yes. Iron deficiency without anemia is common, particularly in:
- Women with heavy menstrual bleeding
- Endurance athletes
- Pregnant women
- Individuals with gastrointestinal disorders
Low ferritin levels can cause fatigue, cognitive impairment, and hair loss even when hemoglobin remains within the normal range.
How low does ferritin have to be to cause symptoms?
Symptoms may appear when ferritin falls below 30 ng/mL, though some individuals experience fatigue or hair shedding at levels below 50 ng/mL.
Clinical interpretation varies based on age, inflammation status, and underlying conditions.
What causes iron deficiency in adults?
The most common causes include:
- Heavy menstrual bleeding
- Gastrointestinal blood loss (ulcers, colon polyps, cancer)
- Pregnancy
- Malabsorption (celiac disease, bariatric surgery)
- Chronic inflammatory conditions
- Insufficient dietary intake
In men and postmenopausal women, unexplained iron deficiency should prompt gastrointestinal evaluation.
How is iron deficiency diagnosed?
Diagnosis typically includes:
- Ferritin (most important marker of iron stores)
- Serum iron
- Total iron-binding capacity (TIBC)
- Transferrin saturation
- Complete blood count (CBC)
Low ferritin confirms iron deficiency unless significant inflammation is present.
How long does it take to recover from iron deficiency?
Recovery depends on severity:
- Energy improvement: 2–4 weeks
- Hemoglobin normalization: 6–8 weeks
- Iron store repletion: 3–6 months
Treatment should continue for at least 3 months after normalization of hemoglobin.
Does iron deficiency cause hair loss?
Yes. Iron supports hair follicle growth. Low ferritin has been associated with diffuse hair shedding (telogen effluvium). Hair regrowth may occur after iron stores are restored.
Can iron deficiency cause anxiety or mood changes?
Iron plays a role in neurotransmitter production. Some patients report:
- Irritability
- Anxiety-like symptoms
- Poor concentration
Improvement is often observed after treatment.
When is iron deficiency dangerous?
Iron deficiency becomes medically urgent if symptoms include:
- Chest pain
- Severe shortness of breath
- Fainting
- Rapid heart rate
- Evidence of gastrointestinal bleeding
Severe anemia can strain the cardiovascular system and requires prompt evaluation.
Can iron deficiency exist without anemia?
Yes. Low ferritin may cause symptoms before hemoglobin drops.
Can diet alone fix it?
Mild deficiency may improve with dietary changes, but moderate to severe deficiency usually requires supplementation.
Is iron supplementation safe?
Yes when guided by a clinician. Excess iron can be harmful if misused.
Final Clinical Perspective
Iron deficiency is common—but not benign. It affects physical performance, cognition, pregnancy outcomes, and cardiovascular function.
Early recognition and proper laboratory evaluation are essential.
If you are experiencing fatigue, hair thinning, shortness of breath, or unusual cravings, discuss iron testing with your healthcare provider.
With proper diagnosis and treatment, recovery is highly achievable—and symptoms are often reversible.
Long-Term Prevention, Recurrence Monitoring & When Iron Deficiency Signals a Serious Condition
Iron deficiency is highly treatable. However, in many patients, it is not a one-time event. Without identifying and correcting the underlying cause, recurrence is common.
A comprehensive care plan does not end when hemoglobin normalizes. It transitions into prevention, monitoring, and appropriate investigation of warning signs.
This final section explains how to prevent recurrence and when iron deficiency requires urgent or advanced medical evaluation.
Will Iron Deficiency Come Back?
It can — particularly if the underlying cause remains unresolved.
Recurrence is more likely in patients with:
- Heavy menstrual bleeding
- Gastrointestinal disorders
- Chronic inflammatory diseases
- Pregnancy or closely spaced pregnancies
- Bariatric surgery history
- Endurance training
- Poor dietary intake
Iron therapy replaces what has been lost. It does not always eliminate the reason iron was lost.
That distinction is clinically important.
Long-Term Prevention Plan
A structured prevention strategy includes dietary optimization, laboratory monitoring, and addressing ongoing sources of blood loss.
1. Maintain Adequate Iron Intake
Iron balance depends on consistent intake and absorption.
Focus on:
- Lean red meat, poultry, fish (heme iron, best absorbed)
- Legumes, spinach, fortified grains (non-heme iron)
- Vitamin C intake with meals to enhance absorption
- Avoiding excessive tea or coffee with iron-rich meals
Patients following vegetarian or vegan diets should discuss supplementation strategies with their clinician.
Diet alone may maintain normal levels after correction, but moderate to severe deficiency often requires ongoing low-dose supplementation.
2. Structured Laboratory Monitoring
Follow-up testing prevents silent relapse.
Typical Monitoring Schedule
- 4–8 weeks after treatment completion
- 3–6 months later if high-risk
- Annually in stable patients with prior deficiency
High-risk patients may require more frequent monitoring.
Labs to Recheck
- Hemoglobin
- Ferritin
- Transferrin saturation
Monitoring ferritin is especially important because iron stores may deplete before anemia redevelops.
3. Address Ongoing Blood Loss
Prevention requires source control.
For Women with Heavy Menstrual Bleeding
Evaluation may include:
- Hormonal therapy
- IUD placement
- Gynecologic consultation
For Gastrointestinal Causes
Evaluation may include:
- Endoscopy
- Colonoscopy
- Testing for celiac disease
- Inflammatory bowel disease assessment
Without treating the source, iron deficiency will recur.
4. Special Populations Requiring Ongoing Monitoring
Pregnancy
Iron needs increase significantly. Even women with normal iron levels before pregnancy may develop deficiency.
Adolescents
Rapid growth increases iron requirements.
Endurance Athletes
Repetitive microtrauma and increased iron turnover may lower ferritin.
Post-Bariatric Surgery Patients
Reduced absorption requires long-term monitoring and sometimes periodic IV iron.
Clinical Case Example: Recurrent Iron Deficiency
A 37-year-old woman treated successfully with oral iron for iron deficiency returns one year later with fatigue.
Ferritin is again low.
Further evaluation reveals untreated heavy menstrual bleeding. After gynecologic management and preventive iron supplementation, recurrence stops.
This case illustrates that long-term success requires identifying the root cause.
When Iron Deficiency Is a Red Flag
Iron deficiency is common in women of reproductive age. However, in certain populations, it should never be dismissed as routine.
Iron Deficiency in Men
Iron deficiency in adult men is uncommon without blood loss.
It warrants evaluation for:
- Gastrointestinal bleeding
- Peptic ulcers
- Colon polyps
- Colorectal cancer
- Inflammatory bowel disease
Unexplained iron deficiency in men should prompt further investigation.
Iron Deficiency After Menopause
Postmenopausal women no longer lose iron through menstruation.
Iron deficiency in this group requires evaluation for:
- Occult gastrointestinal bleeding
- Malignancy
- Chronic inflammatory conditions
Assuming dietary deficiency alone may delay diagnosis of serious disease.
Persistent Iron Deficiency Despite Treatment
If ferritin fails to improve despite adherence:
Consider:
- Malabsorption disorders (celiac disease)
- Chronic inflammation (elevated hepcidin)
- Ongoing hidden blood loss
- Incorrect dosing
- Poor supplement absorption
This situation requires further clinical evaluation.
Iron Deficiency with Additional Concerning Symptoms
Immediate medical assessment is recommended if iron deficiency is accompanied by:
- Unintentional weight loss
- Black or tarry stools
- Rectal bleeding
- Severe abdominal pain
- Persistent vomiting
- Night sweats
- Severe chest pain
These symptoms may indicate serious underlying pathology.
Iron Overload Risk: Avoid Self-Treatment
While deficiency is common, excessive iron supplementation can cause harm.
Iron overload may result in:
- Liver injury
- Oxidative stress
- Organ damage
Iron supplementation should always be:
- Based on laboratory confirmation
- Monitored by a clinician
- Adjusted according to ferritin levels
Self-diagnosing and self-supplementing without testing is not recommended.
Long-Term Outcomes with Proper Management
When appropriately treated and monitored:
- Fatigue improves
- Cognitive function normalizes
- Exercise tolerance returns
- Hair shedding stabilizes
- Pregnancy outcomes improve
- Cardiovascular strain decreases
Early detection prevents complications.
Iron deficiency is highly reversible when managed correctly.
Final Clinical Perspective
Iron deficiency is not simply “low iron.” It is a physiologic condition affecting oxygen transport, neurological function, immune health, and cardiovascular stability.
Treatment is effective. However, long-term success depends on:
- Identifying the underlying cause
- Completing full iron repletion
- Monitoring ferritin levels
- Preventing recurrence
- Recognizing red flags early
If symptoms persist or recur, further medical evaluation is essential.
Comprehensive care transforms iron deficiency from a recurring burden into a manageable, preventable condition.