Skin Cancer Warning Signs: Quick Medical Overview
Skin cancer is one of the most common cancers worldwide, but it is also among the most treatable when detected early. Recognizing the warning signs — including changes in moles, new skin growths, or sores that do not heal — can significantly improve treatment outcomes and survival rates.
Many people assume skin cancer only affects individuals with fair skin or heavy sun exposure. However, medical evidence shows that skin cancer can develop in people of all skin tones and may appear in areas that receive little sunlight, including the soles of the feet, under nails, and genital regions.
This comprehensive medical guide explains:
- Early warning signs of melanoma and non-melanoma skin cancers
- What suspicious moles look like
- When to see a dermatologist
- Risk factors and causes
- Diagnosis and treatment options
- Prevention strategies supported by clinical evidence
Early detection is critical. When melanoma is identified before spreading, survival rates exceed 99 percent.
Quick Facts: Skin Cancer Warning Signs and Early Detection
Medical Topic: Skin Cancer Symptoms, Melanoma Detection, Dermatology Screening
Skin cancer is the most common form of cancer globally, but early detection significantly improves treatment outcomes. Recognizing suspicious skin changes — including new growths, evolving moles, or non-healing sores — is critical for early diagnosis and successful treatment.
Key Warning Signs
- A new mole or skin growth that appears after age 30
- Changes in an existing mole (size, color, shape, or texture)
- A sore that does not heal within 3–4 weeks
- A lesion that bleeds, crusts, or scabs repeatedly
- A shiny, pearly bump or scaly red patch
- A dark streak under a fingernail or toenail
- A spot that looks different from other moles (“ugly duckling” sign)
The ABCDE Rule for Melanoma
Dermatologists recommend checking moles using the ABCDE criteria:
- A — Asymmetry: One half does not match the other
- B — Border: Irregular or poorly defined edges
- C — Color: Multiple colors or uneven pigmentation
- D — Diameter: Larger than 6 mm (may be smaller)
- E — Evolving: Any change over time
Change or evolution is the most important warning sign.
When to See a Dermatologist
Seek medical evaluation promptly if you notice:
- Rapid changes in a mole or skin lesion
- Persistent itching, pain, or tenderness
- A non-healing wound
- Bleeding skin growth
- New pigmented streaks under nails
Early dermatology screening and skin biopsy can detect cancer before it spreads.
Types of Skin Cancer
- Basal Cell Carcinoma: Most common, usually slow growing
- Squamous Cell Carcinoma: Can invade deeper tissues if untreated
- Melanoma: Most aggressive form with higher risk of metastasis
When melanoma is diagnosed early, survival rates exceed 99 percent.
Major Risk Factors
- Ultraviolet (UV) radiation exposure from sunlight or tanning beds
- History of sunburns, especially in childhood
- Fair skin, freckles, or light-colored eyes
- Family or personal history of skin cancer
- Weakened immune system or immunosuppressive medications
- Large numbers of moles or atypical moles
People of all skin tones can develop skin cancer.
Prevention Strategies
- Daily broad-spectrum sunscreen (SPF 30 or higher)
- Protective clothing and sun avoidance during peak hours
- Avoid indoor tanning devices
- Monthly skin self-examinations
- Regular dermatologist skin checks for high-risk individuals
Clinical research shows consistent sun protection reduces skin cancer risk.
Prognosis and Outcomes
Most skin cancers are highly treatable when detected early. Delayed diagnosis increases the risk of invasive disease, complex treatment, and metastasis.
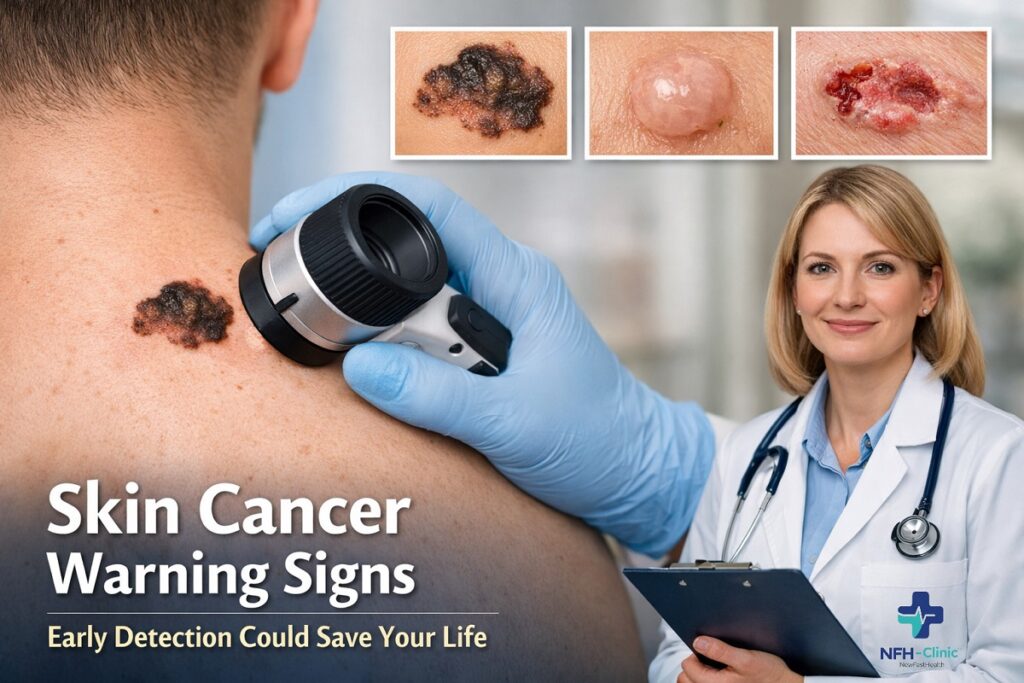
Skin Cancer Warning Signs: Early Symptoms, Pictures to Watch For, and When to See a Doctor
Skin cancer is the most common form of cancer worldwide, but it is also one of the most preventable and treatable when detected early. Recognizing the warning signs can dramatically improve outcomes. Many patients delay evaluation because early symptoms are painless or subtle, which is why education is critical.
This comprehensive guide explains how to recognize skin cancer early, what symptoms require medical attention, and how risk factors influence disease development.
Medically Reviewed Information | NFH Clinic
This article is based on clinical dermatology guidelines, oncology research, and evidence-based prevention recommendations. It is intended for educational purposes and does not replace professional medical advice.
If you notice concerning skin changes, consult a qualified healthcare professional promptly.
What Is Skin Cancer?
Skin cancer occurs when abnormal skin cells grow uncontrollably due to damage in their DNA. This damage is most often caused by ultraviolet (UV) radiation from sunlight or tanning devices, although genetics and immune system factors also play a role.
Skin cancer develops when mutations occur in the DNA of skin cells, causing them to grow uncontrollably. These abnormal cells may invade nearby tissues and, in some cases, spread to other parts of the body (metastasis).
Ultraviolet (UV) radiation from sunlight or tanning beds is the primary environmental cause. However, genetics, immune system function, and environmental exposures also influence risk.
There are three major categories of skin cancer:
- Basal cell carcinoma — most common and usually slow growing
- Squamous cell carcinoma — may grow deeper and spread if untreated
- Melanoma — less common but more aggressive and life-threatening
Early detection dramatically improves treatment success across all types.
1. Basal Cell Carcinoma (BCC)
- Most common type
- Usually slow-growing
- Rarely spreads to distant organs
- Highly treatable when detected early
2. Squamous Cell Carcinoma (SCC)
- Second most common
- Can grow deeper into tissues if untreated
- Higher risk in people with weakened immune systems
3. Melanoma
- Less common but most dangerous
- More likely to spread (metastasize)
- Early detection significantly improves survival rates
Clinical evidence shows that when melanoma is diagnosed early (before spread), the 5-year survival rate exceeds 99%.
Early Warning Signs of Skin Cancer
Skin cancer often begins with small, subtle changes. The most important signs include:
- A new spot or growth on the skin
- A mole that changes in size, shape, or color
- A sore that does not heal within 3–4 weeks
- Persistent itching, tenderness, or bleeding
- A scaly or crusted patch
- A shiny or pearly bump
Any lesion that looks different from your other spots should be evaluated.
What Does Skin Cancer Look Like?
Skin cancer does not always appear the same. It may resemble:
- A new mole or dark spot
- A pink or shiny bump
- A scaly patch
- A sore that repeatedly heals and returns
- A lesion that bleeds easily
- A dark streak under a fingernail or toenail
Any spot that looks different from your other marks or changes over time should be evaluated.
Mole vs Melanoma vs Skin Cancer: Key Differences
Understanding the differences between a normal mole, melanoma, and other types of skin cancer can help you recognize when a skin change may require medical evaluation. The comparison below highlights the most important clinical differences.
| Feature | Normal Mole | Melanoma | Other Skin Cancers (Basal Cell & Squamous Cell) |
|---|---|---|---|
| Appearance | Round or oval, uniform color (tan, brown, or black) | Irregular shape, uneven color, multiple shades | Pink, red, pearly, or scaly lesion; may appear as a sore |
| Border | Smooth and well-defined | Irregular, jagged, or blurred edges | May be raised, crusted, or poorly defined |
| Color | Usually one consistent color | Multiple colors (brown, black, red, white, blue) | Flesh-colored, red, or translucent; may have visible blood vessels |
| Size | Usually small and stable | Often larger than 6 mm but can be smaller | Variable size; may gradually enlarge |
| Change Over Time | Remains stable for years | Evolves in size, shape, color, or symptoms | Slowly enlarges or becomes ulcerated |
| Symptoms | Typically painless | May itch, bleed, or become tender | May bleed, crust, itch, or form a non-healing sore |
| Common Locations | Anywhere on body | Sun-exposed areas and sometimes palms, soles, or under nails | Sun-exposed areas like face, ears, neck, scalp, and hands |
| Cancer Risk | Usually benign | Malignant and potentially life-threatening | Malignant but often highly treatable if detected early |
| Medical Evaluation Needed? | Usually not unless changes occur | Urgent dermatology evaluation recommended | Medical evaluation recommended |
| Diagnosis Method | Visual exam if needed | Skin biopsy required for confirmation | Skin biopsy required for confirmation |
| Treatment | Typically none | Surgical removal ± advanced therapies | Surgical removal, Mohs surgery, or other treatments |
| Prognosis | Excellent | Excellent if detected early; serious if advanced | Very high cure rates when treated early |
While comparison charts are helpful, dermatologists rely heavily on specific diagnostic criteria to evaluate suspicious moles. One of the most widely used tools is the ABCDE rule for melanoma detection.
Key Clinical Takeaway
The most important warning sign that distinguishes melanoma or skin cancer from a normal mole is change over time. Any mole or skin lesion that evolves in size, color, shape, or symptoms should be evaluated by a dermatologist.
Early detection through skin examination and biopsy dramatically improves treatment outcomes and survival rates.
The ABCDE Rule for Melanoma Detection
Healthcare professionals commonly use the ABCDE rule to identify suspicious moles:
A — Asymmetry: One half does not match the other
B — Border: Irregular, jagged, or blurred edges
C — Color: Multiple shades (brown, black, red, white, blue)
D — Diameter: Larger than 6 mm (pencil eraser size), though smaller melanomas occur
E — Evolving: Any change in size, shape, color, or symptoms
While diameter larger than 6 millimeters is a traditional warning sign, research shows melanomas can be smaller. The most important factor is evolution or change over time.
Dermatologists consider change the strongest predictor of malignancy.
The “Ugly Duckling” Sign: A Powerful Clue
Many people naturally have multiple moles. The “ugly duckling” concept refers to a spot that looks different from the rest of your moles.
Research shows this method can improve early melanoma detection, particularly in patients with numerous moles.
Warning Signs of Non-Melanoma Skin Cancers
Basal cell and squamous cell cancers often look different from melanomas.
Common features include:
Basal Cell Carcinoma
- Shiny, pearly bump
- Pink or flesh-colored growth
- Visible blood vessels
- Open sore that heals and returns
Squamous Cell Carcinoma
- Rough, scaly patch
- Wart-like growth
- Thickened or crusted lesion
- Persistent ulcer or sore
These cancers may bleed easily or become tender over time.
Patient Example: Changing Mole
A patient noticed a mole on her back becoming darker and slightly raised over several months. It caused no pain, so she delayed evaluation. A dermatologist diagnosed early melanoma during a routine exam. Surgical removal was curative.
This example highlights why painless changes still require medical attention.
Where Skin Cancer Appears on the Body
Most skin cancers occur in sun-exposed areas:
- Face
- Scalp
- Ears
- Neck
- Arms
- Hands
- Legs
However, they can also appear in areas with little sun exposure:
- Under nails
- Palms and soles
- Genitals
- Between toes
- Buttocks
In people with darker skin tones, melanoma more commonly develops in these less sun-exposed areas (acral melanoma).
Patient Case Examples (Clinical Scenarios)
Case Example 1: Early Melanoma Detected
A 42-year-old woman noticed a mole on her shoulder becoming darker and slightly larger over 6 months. It was painless, but different from her other moles. A biopsy confirmed early melanoma. After minor surgery, she required no further treatment and remains cancer-free.
Clinical takeaway: Subtle change without pain can still indicate cancer.
Case Example 2: Non-Healing Facial Lesion
A 67-year-old man had a small scab on his nose that repeatedly healed and reopened over 2 months. Diagnosis: basal cell carcinoma. Treatment with Mohs surgery achieved complete cure.
Clinical takeaway: A “sore that won’t heal” is a major red flag.
Case Example 3: Skin Cancer in Darker Skin
A 55-year-old patient with dark skin developed a dark streak under a toenail. It was initially thought to be trauma but later diagnosed as melanoma.
Clinical takeaway: Skin cancer affects all skin tones and may appear in unexpected locations.
Causes and Risk Factors
The primary cause is ultraviolet (UV) radiation exposure, which damages DNA inside skin cells.
Risk factors include:
- Frequent sun exposure or tanning bed use
- History of blistering sunburns (especially childhood)
- Fair skin, freckles, or light eyes
- Family history of skin cancer
- Personal history of skin cancer
- Weakened immune system
- Organ transplant medications
- Certain genetic syndromes
- Exposure to radiation or chemicals (e.g., arsenic)
Important note: Anyone, regardless of skin color, can develop skin cancer.
Who Is Most at Risk?
You may have increased risk if you:
- Have fair skin, freckles, or light hair
- Experience frequent sunburns
- Use tanning beds
- Have many moles
- Have a family history of melanoma
- Have a weakened immune system
- Take immunosuppressive medications
- Have had previous skin cancer
However, skin cancer can occur in anyone, including individuals with darker skin tones.
When to See a Doctor
You should seek medical evaluation if you notice:
- A new mole after age 30–40
- Any changing lesion
- A sore that does not heal within 4 weeks
- Bleeding or crusting skin growth
- Persistent itching or pain in a spot
- Dark streak under a nail
Early evaluation often requires only a simple skin exam or biopsy.
How Skin Cancer Is Diagnosed
Doctors typically use:
- Visual skin examination
- Dermoscopy (magnified skin imaging)
- Skin biopsy (definitive diagnosis)
Biopsy is quick, usually done with local anesthesia, and is essential for accurate diagnosis.
Treatment Outcomes and Prognosis: What to Expect After a Skin Cancer Diagnosis
Treatment for skin cancer is highly individualized and depends primarily on the type of cancer, tumor size, location, depth of invasion, and whether the disease has spread (stage). Fortunately, most skin cancers are very treatable, especially when detected early, and many patients achieve complete cure with minimally invasive procedures.
Understanding treatment options and expected outcomes can help reduce anxiety and support informed decision-making.
First-Line Treatment: Surgical Removal
For most skin cancers, surgical excision is the primary and most effective treatment. During this procedure, a physician removes the cancer along with a small margin of surrounding healthy tissue to ensure complete removal.
Clinical outcomes:
- Cure rates are extremely high for early basal cell and squamous cell cancers.
- Early melanoma treated surgically often requires no additional therapy.
- Recurrence risk is low when margins are clear.
For many patients, this is an outpatient procedure performed under local anesthesia with minimal recovery time.
Mohs Micrographic Surgery (Precision Cancer Removal)
Mohs surgery is considered the gold standard for certain skin cancers, particularly those located on cosmetically sensitive areas such as the face, ears, or nose.
This technique removes cancer layer by layer while immediately examining tissue under a microscope to confirm complete removal.
Advantages include:
- Highest cure rates (often above 95–99%)
- Maximum preservation of healthy tissue
- Reduced scarring compared with traditional surgery
- Lower recurrence rates
Mohs surgery is especially valuable for recurrent tumors or cancers with poorly defined borders.
Cryotherapy (Freezing Treatment)
Cryotherapy uses extreme cold (usually liquid nitrogen) to destroy abnormal skin cells.
It is typically used for:
- Very early or superficial skin cancers
- Precancerous lesions such as actinic keratosis
While effective for selected cases, deeper or aggressive cancers usually require surgical treatment instead.
Radiation Therapy
Radiation therapy may be recommended when surgery is not possible or when tumors are located in areas difficult to treat surgically.
It may also be used:
- After surgery to reduce recurrence risk
- For advanced cancers
- In older adults who cannot undergo surgery
Radiation therapy is noninvasive but typically requires multiple treatment sessions over several weeks.
Advanced Treatments for Melanoma and High-Risk Skin Cancer
When skin cancer spreads beyond the original site, more advanced therapies may be required.
These include:
Immunotherapy
Immunotherapy medications stimulate the body’s immune system to recognize and destroy cancer cells.
This approach has significantly improved survival in advanced melanoma and some high-risk skin cancers.
Targeted Therapy
Targeted therapies focus on specific genetic mutations within cancer cells, allowing more precise treatment with fewer effects on healthy tissues.
These treatments are often used when melanoma carries certain genetic markers.
Clinical research has dramatically improved survival outcomes in patients with advanced melanoma using these therapies.
Treatment Outcomes: What the Evidence Shows
Prognosis varies widely depending on how early cancer is detected.
Strong clinical evidence demonstrates:
- Early-stage skin cancers have extremely high cure rates.
- Melanoma detected before spread has survival rates greater than 99%.
- Non-melanoma skin cancers rarely become life-threatening when treated promptly.
- Delayed diagnosis increases the risk of deeper invasion, metastasis, and more complex treatment.
In practical terms:
Early detection often means minor surgery and complete cure.
Late detection may require extensive treatment and carries higher health risks.
Patient-Centered Perspective: Recovery and Quality of Life
Most patients treated for early skin cancer:
- Return to normal activities quickly
- Experience minimal discomfort
- Require only routine follow-up monitoring
Even patients with more advanced disease now have more treatment options than ever before due to advances in oncology and immunotherapy.
Regular follow-up appointments remain essential because individuals who develop skin cancer once have a higher risk of developing another in the future.
Key Takeaway
Skin cancer outcomes are strongly linked to how early the cancer is diagnosed and treated. Prompt medical evaluation of suspicious skin changes offers the best chance for simple treatment, minimal scarring, and complete recovery.
Prevention: How to Reduce Your Risk
Prevention strategies are strongly supported by medical research.
Sun Protection Measures
- Use broad-spectrum sunscreen SPF 30 or higher daily
- Reapply every 2 hours outdoors
- Wear protective clothing and hats
- Seek shade during peak sun hours (10 a.m. to 4 p.m.)
- Avoid tanning beds completely
Even on cloudy days, UV exposure occurs.
Clinical studies show that consistent sunscreen use significantly reduces the risk of melanoma and non-melanoma skin cancers.
When to See a Dermatologist
You should schedule a medical evaluation if you notice:
- A mole that changes in size, color, or shape
- A new growth after age 30
- A sore that does not heal within 3–4 weeks
- Bleeding or crusting lesions
- Persistent itching or tenderness
- Dark streaks under nails
Early consultation often leads to simpler treatment and better outcomes.
How to Perform a Monthly Skin Self-Exam
A full skin check takes about 10 minutes.
Steps:
- Check face, ears, neck, and scalp
- Examine arms, hands, and under nails
- Look at chest and torso
- Inspect legs and feet (including soles)
- Use mirrors for back and buttocks
- Check genital area
Document any changes with photos if possible.
Frequently Asked Questions About Skin Cancer
What are the first signs of skin cancer?
The earliest signs often include a new skin growth, a mole that changes in size or color, or a sore that does not heal within several weeks. Some skin cancers appear as shiny bumps, scaly patches, or lesions that bleed easily.
Change over time is one of the most important warning signals.
What does melanoma look like in the early stages?
Early melanoma may appear as an unusual mole with irregular borders, uneven color, or asymmetry. It may also look different from your other moles, which is known as the “ugly duckling” sign.
Not all melanomas are dark. Some may be pink, red, or skin-colored.
Can skin cancer be itchy?
Yes. Skin cancer can sometimes cause itching, tenderness, or irritation. However, many skin cancers cause no symptoms at all, which is why visual changes are important to monitor.
Is skin cancer painful?
Most early skin cancers are painless. Pain usually develops later if the cancer grows deeper or becomes inflamed. Lack of pain does not mean a lesion is harmless.
How fast does melanoma spread?
Melanoma growth rates vary. Some grow slowly over months or years, while others may spread more rapidly. Early detection before spread dramatically improves survival rates.
Can people with dark skin get skin cancer?
Yes. Skin cancer can occur in all skin tones. In individuals with darker skin, melanoma often appears on the palms, soles, under nails, or mucous membranes rather than sun-exposed areas.
When should I see a doctor about a mole?
You should seek medical evaluation if a mole:
- Changes in size, color, or shape
- Bleeds or crusts
- Becomes itchy or painful
- Looks different from other moles
- Appears after age 30–40
Can skin cancer go away on its own?
No. Skin cancer does not resolve without treatment. Delaying medical care may allow the cancer to grow or spread.
How is skin cancer diagnosed?
Diagnosis usually involves a skin examination followed by a biopsy, where a small sample of tissue is removed and analyzed under a microscope.
A biopsy is the only definitive way to confirm skin cancer.
What is the survival rate for skin cancer?
When detected early, most skin cancers have very high cure rates. Early melanoma has a survival rate greater than 99 percent. Advanced melanoma has lower survival rates, which is why early detection is critical.
Evidence-Based Medical Notes
- UV radiation is classified as a Group 1 carcinogen.
- Indoor tanning increases melanoma risk significantly, especially before age 35.
- Regular skin checks improve early detection rates and survival outcomes.
- Mohs surgery offers cure rates above 95% for many non-melanoma cancers.
Key Takeaways
- Watch for new, changing, or unusual skin spots.
- Use the ABCDE rule and ugly duckling sign.
- Non-healing sores require evaluation.
- Early detection dramatically improves survival.
- Prevention through sun protection is highly effective.
Skin cancer is common but often preventable and highly treatable when detected early. Becoming familiar with your skin and recognizing warning signs can save your life.
If you notice suspicious changes, seeking prompt medical evaluation is one of the most important health decisions you can make.